Does Your Team Utilize Gabapentin Appropriately?
A survey of 718 North American veterinarians reveals widespread misunderstanding of gabapentin’s mechanism of action and frequent inappropriate prescribing for acute pain and as a sole analgesic.

Does your team utilize gabapentin appropriately? Do you understand how gabapentin works (the mechanism of action)? Do you know when & why to use gabapentin for your patients?
Objective
Determine how gabapentin is currently being utilized and prescribed as an analgesic by North American (USA & Canada) veterinary practitioners.
Study Design
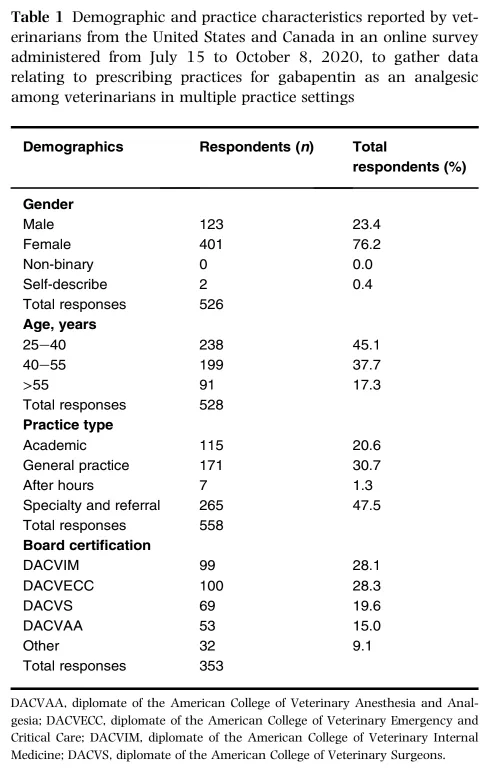
Anonymous survey to veterinarians in North America (n = 718 respondents) over a 4-month period. General Practice & Specialty Practice surveyed. Specialties included: anesthesiology, critical care, surgery, internal medicine, sports med/rehab, nutrition, dermatology, lab animal, and various ABVP.
Consider: does the timeframe for responses impact results?
The voluntary survey was shared via email to professional listservs for veterinary specialties (ACVAA, ACVECC, ACVIM, ACVS), other various veterinary organizations (e.g. Veterinary Orthopedic Society), two state VMAs, and social media platforms.
Consider: does the method of survey distribution potentially alter the demographics of respondents and could that alter results?
Questions asked focused on gabapentin’s mechanism of action, perceived efficacy, and perceived human abuse potential: gabapentin’s pharmacologic properties, the respondent’s veterinary demographics (e.g. practicing sector of vet med), frequency of gabapentin use, and reason for gabapentin prescription.
Survey required respondents to select their choice from a set of answer options.
Consider: could multiple-choice answers possibly lead to bias? Would open-response answers potentially provide more accurate responses?
Results
Respondents:
- Only 74% of respondents answered the entire survey
- Majority of respondents (92%) worked with Small Animal species
- Approximately ⅓ of respondents worked as General Practitioners (30%), whereas the majority of respondents worked as Specialists (63%)
Consider: do the demographics of general practitioners vs specialists as respondents impact the results?
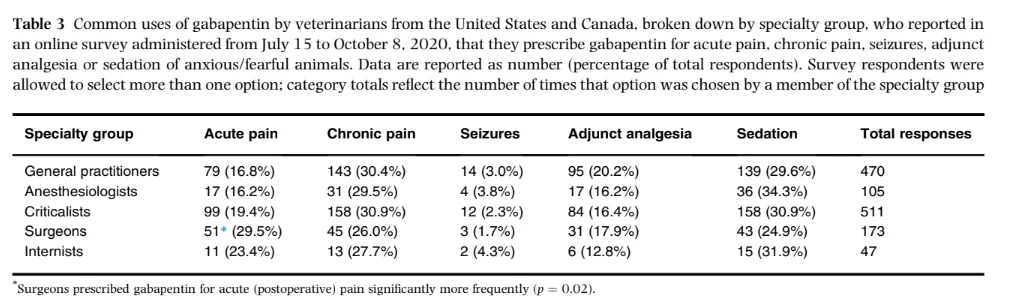
Frequency of gabapentin use = 97% of all respondents. Over 70% prescribed on daily to weekly basis. Surgeons + GPs prescribed gabapentin significantly more frequently than all other practitioners.
Reason(s) for prescribing gabapentin:
- Alternative analgesic when NSAIDs contraindicated (50% of all respondents) — most common reason among Anesthesiologists
- Thought gabapentin was the appropriate or most effective analgesic (32% of all respondents) — most common reason among Surgeons + Internists
Intention(s) behind gabapentin use:
- Acute / post-operative pain — significantly more frequently chosen by Surgeons compared to all other respondents
- Chronic pain — chosen by approximately ⅓ of respondents from each category
- Seizures
- Sedation
- Chosen as the sole analgesic significantly more frequently by GPs, Surgeons, Criticalists compared to Anesthesiologists
Practitioners and understanding of gabapentin’s mechanism of action (MOA):
- Only 44% of all respondents correctly identified gabapentin’s MOA
- 35% of respondents incorrectly chose gabapentin’s MOA and 20% of respondents indicated they did not know the MOA
- Significant difference in knowledge of gabapentin’s MOA between veterinary anesthesiologists (DACVAA) and all other respondents
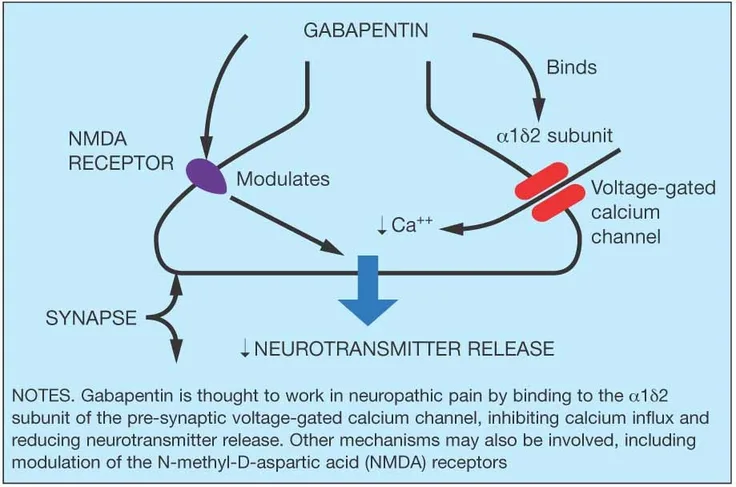
Despite its name and origins during initial discovery of the drug, gabapentin’s mechanism of action is via action at voltage-gated Ca2+ channels and not via alterations of GABA or at GABA-receptors.
Gabapentin primarily works at calcium channels to inhibit release of excitatory/painful neurotransmitters (e.g. glutamate, substance-P). This mechanism mainly provides analgesia for neuropathic & chronic pain. Sedation is a common side effect that many practitioners utilize gabapentin for instead of for its analgesic properties.
Conclusions & Limitations
Despite frequent use, gabapentin is often prescribed inappropriately in regard to its analgesic properties by the majority of veterinarians in North America. Few veterinarians understand gabapentin’s mechanism of action / pharmacology.
- There were significant differences found with how, when, and why Anesthesiologists vs other veterinarians chose to utilize gabapentin
- Despite 50% of Surgeons & Criticalists correctly identifying gabapentin’s MOA, these groups of veterinarians were shown to more likely use gabapentin for inappropriate indications (e.g. acute pain & as sole analgesic)
Consider: how can we help the veterinary community better understand & utilize gabapentin to improve our analgesic management standards across all sectors?
Many veterinarians use gabapentin for analgesia when NSAIDs are contraindicated. Pain is complex and involves various pathways, neurotransmitters, and receptors.
Consider: is gabapentin providing the same method of analgesia as an NSAID?
Sedation is a known side effect of gabapentin that is often desired in some patients.
Consider: do the sedative effects alter our ability to accurately assess pain in these patients?
Limitations — Respondent Bias:
- Method of survey distribution may have gathered veterinarians more inclined, and possibly more knowledgeable on the subject, to respond and determine these results
- General practitioners were only aware of this survey if members of the only 2 state VMAs that were emailed — 2 states does not represent all of the GPs in North America
- Unequal distribution of respondents from each specialty group
- Questions may have been ambiguous and/or the multiple-choice answers may have created bias — may have resulted in poor survey completion rates
Be more intentional with gabapentin use: gabapentin is not appropriate for acute or post-surgical pain. It is best indicated for chronic or neuropathic pain processes due to its mechanism of Ca2+ channel alterations (not via GABA). Gabapentin is not interchangeable for NSAID analgesia. It is best used as an adjunct analgesic (not the sole analgesic). Gabapentin’s sedative qualities are sometimes beneficial, however this should not mask our ability to accurately assess pain.
Want to Learn More?
Whether you're looking for hands-on training or expert consultation, MACvet™ is here to support your team and your patients.