Facemask vs Flow-By: Which Preoxygenation Method Is More Effective?
A crossover study of 6 dogs compares facemask vs flow-by preoxygenation methods, revealing significant differences in oxygenation variables and time to desaturation before anesthetic induction.

Are you curious if the way your team provides O2 supplementation is effective or best-practice? Does your team preoxygenate your pre-anesthetic patients? Should you? How does your team provide O2 supplementation? What scenarios & what patients benefit from preoxygenation?
Objective
Is there a difference in how long it takes a patient to desaturate (i.e. drop in SpO2 to 90%) when providing oxygen via two different methods: facemask vs flow-by?

Study Design
Same dog (n = 6) anesthetized twice every 2 weeks to receive each of the two treatments: facemask vs flow-by O2.
Crossover Design — avoids results-variability due to differences in each individual. n = 6 is a very small sample size; this is common in vet medicine (compared to human medicine) due to accessibility issues — Study Limitation!
Dogs were sedated to place intratracheal catheter for sampling of tracheal oxygenation variables (FiO2 — inspired O2 % and FeO2 — expired O2 %).
Dogs received same protocol for each treatment — avoids results-variability due to drug differences: dexmedetomidine + acepromazine + butorphanol IM.
Dogs were preoxygenated at the nares for 3 minutes either via facemask or flow-by prior to anesthesia. Other studies have shown adequate preoxygenation requires at least 3 minutes to be effective. O2 flow rate 100 mL/kg/min via Circle Y-Piece circuit.
Anesthesia was induced with propofol until apnea occurred. Time to desaturation from induction was measured until 90% SpO2 reached and dogs were then intubated to allow for adequate oxygenation + ventilation.
Pulse oximetry was measured lingually.
Consider: does SpO2 site matter?
Variables assessed: time to desaturation (seconds) at SpO2 = 90%, FiO2 + FeO2 (%) — content % of oxygen being inspired & expired, SpO2 (%) — prior to and after O2 supplementation, PaO2 (mmHg arterial blood O2) — prior to O2 supplementation, 5 sec post-induction, and every 30 sec until desaturation point reached.
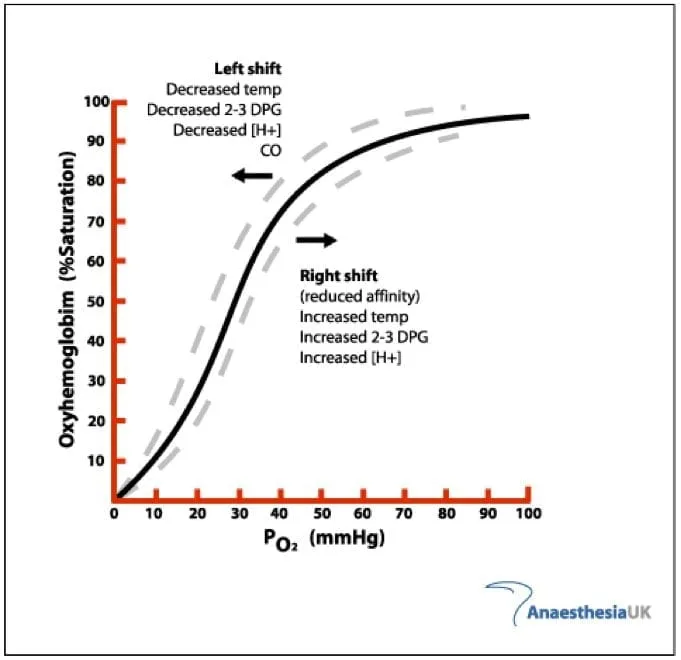
Consider: how do each of these variables relate to oxygenation status?
Results
Oxygenation variables (FiO2, FeO2, and PaO2) were significantly higher in dogs receiving facemask preoxygenation compared to flow-by method:
- Facemask Dogs: FiO2 = 90%, FeO2 = 83%, PaO2 = 390mmHg
- Flow-by Dogs: FiO2 = 30%, FeO2 = 23%, PaO2 = 130mmHg
Consider: despite the fact that the FiO2 = 100% from a medical circuit (remember: room air = 21% O2), what O2 % the patient actually inspires into their respiratory tract is dependent on how much of that 100% is saturated around their respiratory structures (e.g. nares & oropharynx). Method of delivery is a factor — facemask delivers 3x the O2 % compared to Flow-by method (delivers barely above room air O2 %).
Time to desaturation (SpO2 = 90%) took significantly longer to reach in dogs preoxygenated via facemask compared to flow-by method:
- Facemask Dogs: desaturation time = 190 seconds (3 min)
- Flow-by Dogs: desaturation time = 65 seconds (1 min)
Consider: those extra 120 seconds (2 minutes) can make a huge difference in how quickly a patient reaches critically low oxygenation status.
Preoxygenation is extremely important in all cases (including sedations), but especially in the following scenarios:
- Difficult intubations — cat laryngospasms, brachycephalics, oropharyngeal masses, jaw abnormalities, certain species (e.g. rabbits/camelids/swine)
- Reduced FRC (functional residual capacity) — obesity, abdominal mass effects (e.g. pregnancy, effusion, hepatomegaly or mass)
Conclusions & Limitations
Facemask preoxygenation was superior to the flow-by method in preventing desaturation (SpO2 = 90%). Facemask preoxygenation is more effective in preventing apneic patients from reaching critically low oxygenation status.
Common Concern: “My patient isn’t tolerating the facemask. How do I preoxygenate effectively then?”
- Almost all patients will tolerate facemask preoxygenation if properly sedated — it is crucial for certain cases that they are preoxygenated properly!
- Did we sedate this patient appropriately? Consider: appropriate drug combo or dose for patient?
- Did we allow enough time for sedation protocol to work? Consider: do you know the normal onset time for your drugs & how route of administration may impact that onset time?
Limitations:
- Small sample size — larger sample size would help support these findings if same results also found in more individuals receiving the same treatment
- CV parameters (not assessed in this study) & site of arterial blood gas measurement may impact PaO2 values
Make sure to preoxygenate ALL patients with a facemask for gold-standard anesthesia care.
Want to Learn More?
Whether you're looking for hands-on training or expert consultation, MACvet™ is here to support your team and your patients.