Are Tongue-Based Oscillometric Blood Pressure Measurements Accurate in Dogs?
A prospective study of 45 anesthetized dogs evaluates whether oscillometric blood pressure measured from the tongue is a reliable alternative to traditional NIBP sites and invasive arterial blood pressure.

Are oscillometric blood pressure measurements accurate when using the tongue as the measuring site in dogs? Is it performed similar to oscillometric-NIBP when measured on appendages (limb and/or tail)? How accurate are the measurements compared to traditional NIBP-oscillometric sites and/or arterial blood pressure?
Objective
Determine if oscillometric-NIBP (O-NIBP) measured from the tongue is a favorable estimate of SAP, MAP, and DAP in anesthetized dogs.
Study Design
Prospective analysis of 45 dogs (n = 45).
- Inclusion criteria = dogs receiving anesthesia that included invasive blood pressure (IBP) monitoring as part of protocol
- No exclusion criteria
Consider: how do different disease states and anesthetic agents impact perfusion to different blood pressure monitoring sites?
- Dogs with any co-morbidity — confounder with individual variability
- Dogs receiving different anesthetic protocols — not standardized = confounder with perfusion variability depending on CV effects of each individual or combination of drugs utilized
- Agents utilized (variable combination used with every dog): acepromazine, midazolam, alfaxalone, isoflurane, remifentanil infusion, lidocaine infusion, ketamine infusion
- Dogs receiving variable anesthesia duration & procedure types — confounder with perfusion variability depending on anesthetic duration and/or procedure being performed
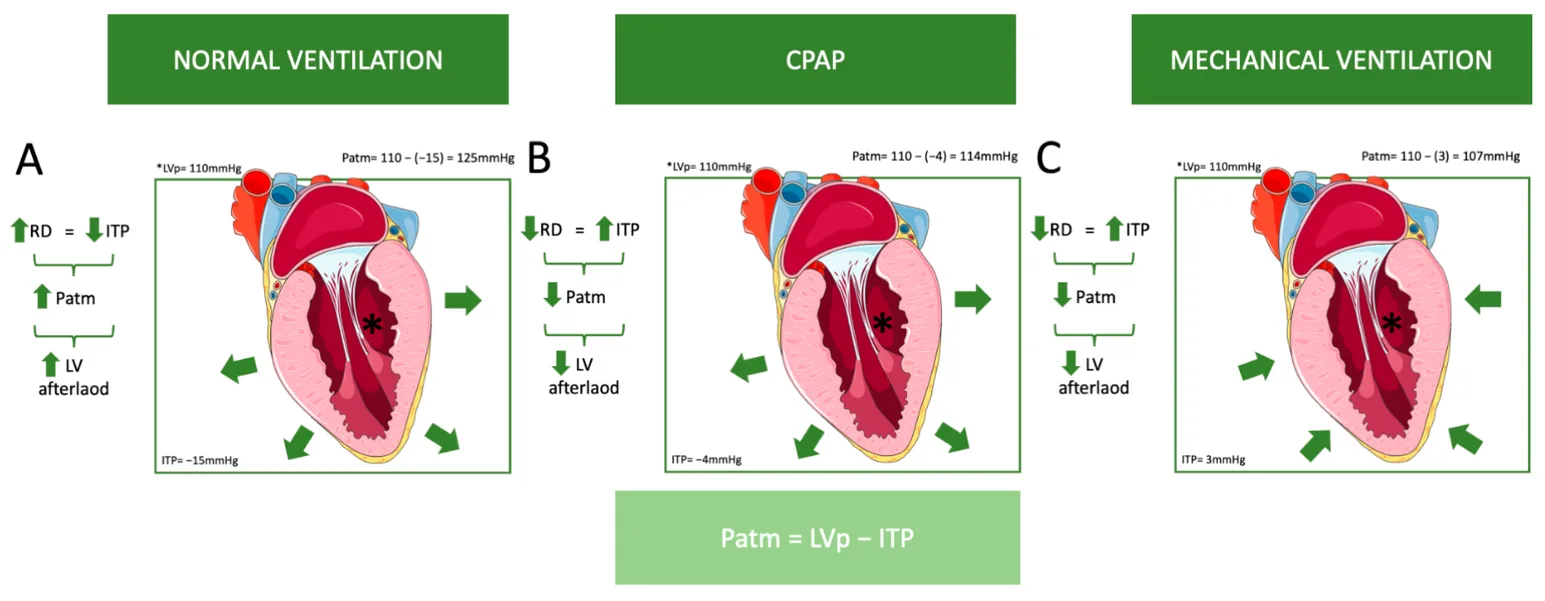
Dogs received controlled mechanical ventilation (CMV) to maintain capnography EtCO2 35–45mmHg.
Consider: how does positive pressure ventilation (PPV) impact perfusion? How do carbon dioxide levels impact blood pressure?
All dogs had an arterial catheter placed in the dorsal pedal artery for IBP monitoring.
Consider: while IBP is gold-standard method of blood pressure measurement, are the values equivalent across different arterial catheter sites? (e.g. dorsal pedal artery vs coccygeal / tail artery)
Other monitoring instituted = ECG, SpO2, spirometry, and esophageal temp.
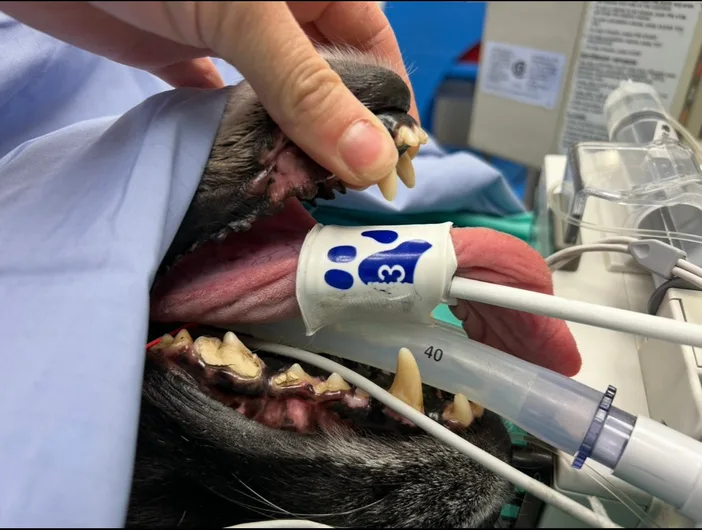
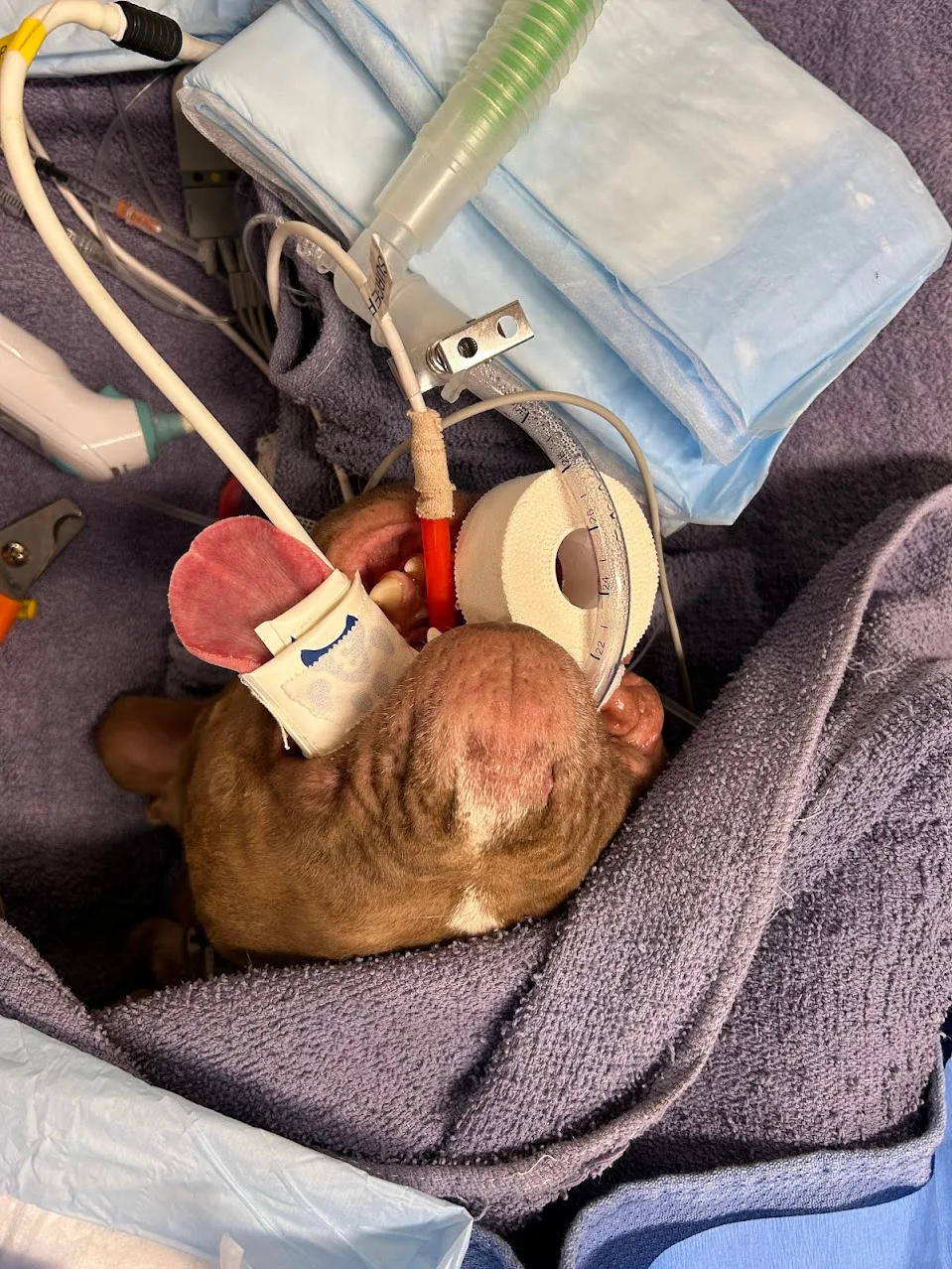
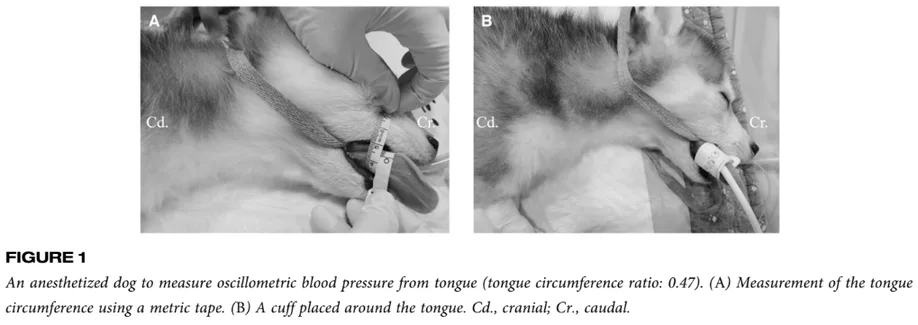
Tongue O-NIBP method:
- BP cuffs positioned rostral to lingual frenulum
- Tongue circumferences measured to calculate tongue circumference ratio
- Utilized traditional 40% ratio recommendations (as per manufacturer cuff size recommendations and ACVIM + AAMI criteria for NIBP measurement)
- Tongue O-NIBP measurements obtained only when IBP measurements within normal systolic blood pressure ranges (SAP 90–139mmHg)
- O-NIBP device was set to either small or large dog based on manufacturer’s recommendations (small dog setting = <8kg)
- O-NIBP and IBP measurements recorded simultaneously and compared: SAP/MAP/DAP-tongue vs SAP/MAP/DAP-arterial
- Initial measurement discarded & subsequent 5 measurement readings recorded for analysis
- Unobtainable readings — cuff repositioned & O-NIBP restarted
Results
Sample size & demographics:
- 45 dogs — relatively small sample size
- Variable ages (1–15yo) — perfusion variabilities exist across life-stages
- Variable weights (2.5–45kg) — measurement accuracy variable with size
- Uneven distribution of dog size: dogs <5kg (n=16/45) vs >5kg (n=29/45) — analysis of results were stratified by body weight (<5kg or >5kg)
- Variable dog breeds
- Variable procedure types: orthopedic = 38%, soft-tissue = 56%, imaging = 6%
- Cuff circumference ratio across all dogs was 0.42 +/- 0.06 — maintained the standard 40% recommendations
- Tongue O-NIBP measurements performed = 225 total measurements — fairly large size for comparison
- Same total amount of IBP measurements
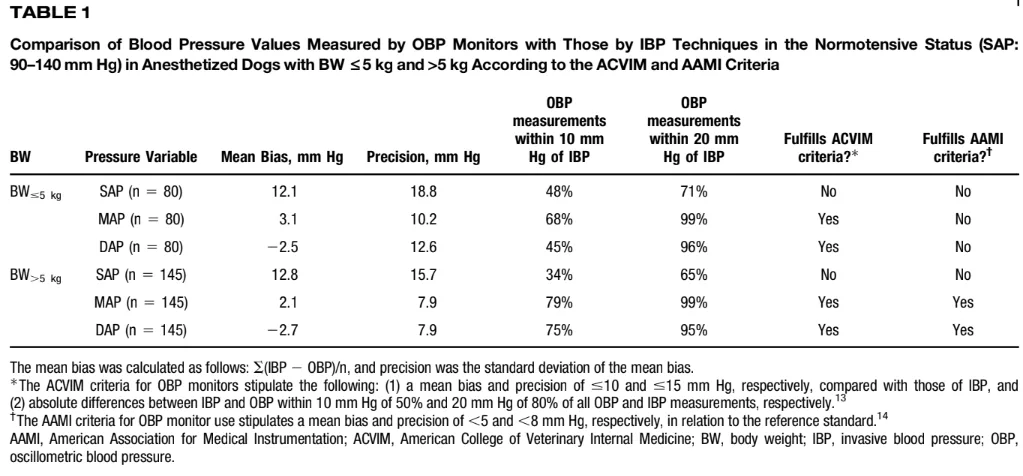
- SAP-tongue for both weight groups underestimated arterial SAP
- SAP-tongue did not meet ACVIM nor AAMI criteria for agreement
- MAP-tongue + DAP-tongue were in agreement with arterial MAP & DAP in the large dog group, but not consistently in the small dog group:
- >5kg group = MAP-tongue + DAP-tongue met both ACVIM & AAMI criteria for agreement
- <5kg group = MAP-tongue + DAP-tongue only met the ACVIM criteria for agreement
Conclusions
When considering ACVIM criteria:
- Both MAP & DAP tongue O-NIBP were clinically interchangeable with arterial/IBP measurements
- SAP-tongue showed poor agreement with arterial SAP measurements — tongue O-NIBP often underestimated arterial SAP measurement
- Poor agreement for systolic BP measurements is a common feature of oscillometric devices even at traditional measurement sites (e.g. limbs)
- Prioritizing the mean BP is often preferred when using oscillometric devices due to proven accuracy of MAP over other BP measurements
When considering AAMI criteria:
- Dogs weighing <5kg exhibited less reliable agreement than dogs >5kg
Consider: is it solely body size or potentially other factors (e.g. specific comorbidities more common in small breed dogs) that may have impacted these results?
Poor agreement with oscillometric measurements in smaller patients (<5kg) has been shown in previous studies as well.

Limitations
- Sample size relatively small — n of 45 is fairly small amount of individuals to represent the entire anesthetized dog population
- Plenty of sample variability: significant confounders present with non-standardized breeds and ages of dogs, anesthetic protocol and duration, & procedure types performed
- Blood pressure measurements only analyzed during normotension ranges — uncertain if these results will hold true in hyper- or hypo-tensive patients
- Measurement sites between O-NIBP and IBP methods not standardized — ideal to compare NIBP vs IBP from the same sampling site, as various body parts have varying perfusion & vascular tone alterations
- Authors also acknowledge that long-term assessment of tongue O-NIBP was not performed in regards to potential injury to either the tongue or vascular supply (confirmed no overt concerns present immediately after anesthesia)
Oscillometric MAP and DAP (but not SAP) measurements acquired from the tongue site is likely a reliable alternative to traditional NIBP sites. It is important to keep in mind that the size of patient may reduce the tongue’s reliability in providing accurate O-NIBP measurements.
Want to Learn More?
Whether you're looking for hands-on training or expert consultation, MACvet™ is here to support your team and your patients.